|
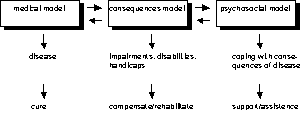
A review of psychosocial models in psychogeriatrics:
|
| Stages | Psychosocial crises | Favorable outcome |
| 1. 1th year | Trust versus mistrust | Trust and optimism |
| 2. 1-2 years | Autonomy versus doubt | Sense of self-control and adequacy |
| 3. 3-5 years | Initiative versus guilt | Initiative versus guilt |
| 4. 6-puberty | Industry versus inferiority | Competence in intellectual, social and physical skills |
| 5. Adolescence | Identity versus confusion | An integrated image of oneself as a unique person |
| 6. Early adulthood |
Intimacy versus isolation | Ability to form close and lasting relationships; to make career commitments |
| 7. Middle adult-hood | Generativity versus self-absorption | Concern for family, society and future generations |
| 8. The aging years | Integrity versus despair | A sense of fulfillment and satisfaction with one’s life; willingness to face death |
In the final development stage of the Erikson developmental stage model ‘integrity versus despair’, people evaluate their lives by reminiscing. Butler describes the importance of looking back on life (life review) for the psychologic well-being of people. He indicates that this becomes increasingly important as people be-come older. It is a natural, spontaneous process, during which one becomes conscious again of past events.
In the psychogeriatric field, Feil (1967, 1984, 1989) and Kihlgren et al. (1996) have applied the Erikson developmental stage model. Feil (1967, 1984, 1989) based her validation approach on elements from the Erikson developmental stage model. Validation is based on the idea that behavior of the elderly is deter-mined not only by the condition of the brain, but also by a number of other physical and psychosocial fac-tors. One of those factors is the degree to which a person has gone through the different stages of develop-ment successfully (Feil, 1992). Feil criticizes Erikson for not taking into account the serious physical losses that occur at an advanced age during the final stage of life (integrity versus despair). Feil and De Klerk-Rubin (1991) indicate that inner harmony (integrity) can only be reached if a person still has the cognitive ability to cope with problems. Therefore, she added a ninth stage to the Erikson developmental stage model. In this ninth stage, ‘resolution versus vegetation’ is the central issue. Adding this stage makes it possible to give more specific attention to disoriented elderly people, who experience relief when validated in their feelings. This is a central aspect of the validation approach.
Kihlgren et al. (1996) used the Erikson developmental stage model as the theoretical framework for the in-tervention and data analyses in research among nursing home residents with severe dementia (N=5). After the staff took part in a training course, aimed at encouraging the inner harmony (integrity) of the residents, interaction between residents and staff increased, and the residents started exhibiting more ‘strong’ char-acteristics, such as: expres-sing hope, their own wills, goals, competence, and trust. The vague description and observability of the ‘weak’ characteristics proved problematic in the application of the Erikson devel-opmental stage model (Kihlgren et al. 1996).
Progressively lowered stress threshold model
Hall and Buckwalter (1987) developed the progressively lowered stress threshold model (PLST model) starting from a balanced interaction between individual and environment. Their model is based on the coping theories of Lazarus (1966) and Selye (1980) and the results from learning theoretical and physiol-ogic research on people with Alzheimer’s disease (Hall, 1994).
The PLST model focuses on the influence of the care environment. The star-ting point is that the environ-ment must be adjusted to fit people with dementia and their deteriorating cognitive and functional abilities (Gerdner et al. 1996).
The model’s target group consists of people with Alzheimer’s disease and related disorders. The model aims to provide a theoretical framework for the individual care of these people, both in the home situation and the institutional setting (Hall et al. 1995b).
The PLST model distinguishes four stages in Alzheimer’s disease: (forgetfulness, confusion, ambulatory dementia, and end stage). The accompanying symptoms consist of: cognitive or intellectual losses; affec-tive or personality changes, conative (concerning the will) losses, planning capability losses and a progres-sively lowered ‘stress threshold’, which may generate dysfunctional behavior (i.e., agitation, repetitive be-havior, wandering, night-time unrest, aggression).
As the disease progresses, the stress threshold is lowered during the course of the day, depending on the stress factors. The stress factors are divided into six categories: (1) fatigue, (2) changes regarding the care-giver, environment or routine, (3) demands that exceed a person’s capabilities, (4) overwhelming and con-flicting stimuli, (5) affective reactions to experienced losses, and (6) physical stressors, such as acute ill-ness or pain. This categorization of stress factors can be used to gather diagnostic data and to plan and evaluate care.
The PLST model has been used extensively in the provision of care for people with Alzheimer’s disease to design individual care programs, modify the environment and, design special treatment programs, and evaluate interventions (Hall, 1988, 1994; Hall & Buckwalter, 1991; Hall et al. 1995a). The model is fur-thermore used as a context for nursing research (Hall, 1994; Collins et al. 1995).
The Dialectical framework
Kitwood (1989, 1990, 1993a, 1993b, 1996, 1997, 1998) starts from a dialectical framework to explain the dementia process. In his opinion, a constant interaction between neurologic disabilities (situation) and so-ciopsychologic processes (causal factor) cause the dementia process. This interaction is responsible for the emergence of a new situation that in turn interacts with causal factors, which again generates a new situa-tion, and so on (Kitwood, 1996).
The dialectical framework was developed from the idea that the biomedical perspective is inadequate when it comes to explaining the dementia process and the clinical dementia picture. Kitwood does not dismiss the biomedical paradigm, but views the symptomatology of elderly people with dementia as a result of the interaction between various factors (i.e., personality, life history, physical health, neurologic damage, and the sociopsychologic environment).
Personality, life history and progressing neurologic damage are presumed to be ‘facts’ that are difficult to influence. Physical health, social psychology, and the way the person is approached by others then remain as crucial factors that can be influenced. Regarding physical functioning, an improvement in physical functions is frequently accompanied by an improvement in mental health (Kitwood, 1993a).
As the brain increasingly degenerates and inner stability decreases, psychologic functioning becomes in-creasingly susceptible to negative environmental influences. That is why it is important that an environ-ment is created that offers sufficient stability and love to enable the person with dementia to maintain the highest possible level of psychologic functioning.
Within the sociopsychologic environment, behaviors are distinguished that may have a negative impact on the person with dementia, such as: treating the person as a child, taking over activities unnecessarily, and ignoring the dementing person’s feelings (Kitwood, 1990; 1993a). However, there are also approaches that may have a positive effect on the well-being and functioning of the person with dementia, for example: of-fering a safe environment, accepting the way the person experiences the world, enabling the person to do things they would otherwise be unable to do, and stimulating the senses (Kitwood, 1996).
A purely scientific verification of the Kitwood model is difficult, because the subject matter is too complex and the theory is too vague (Kitwood, 1990). It is, however, possible to examine the effect of a positive or negative approach on the person with dementia by means of dementia care mapping (DCM). Dementia care mapping is an observational technique that entails indicating what happens to the elderly person with dementia and the degree of his well-being during a set time in consecutive periods of 5 minutes. One hundred ten aspects are distinguished (i.e., sleeping, walking, receiving physical care); in addition, negative behaviors by people in the environment of the person with dementia have been operationalized into 30 categories.
Kitwood indicates that his starting points apply to both the home situation and to institutional settings. We were not able to determine to what extent the model is being applied in practice and research outside the dementia care mapping studies conducted by Kitwood (Kitwood & Bredin, 1992; 1994) and by Spaull and Leach (1998) who used dementia care mapping in their evaluation of the effects of sensory stimulation on people who have dementia.
Attachment theory
Miesen (1990, 1992, 1997) used the attachment theory developed by Bowlby (1983) as an explanatory model regarding parent-fixation in elderly people with dementia.
Bowlby (1983) states that attachment behavior consists of all behaviors that focus on the proximity of an ‘attachment figure’, who is another person. Attachment behavior induces the attachment figure to exhibit care behavior. Attachment behavior is present or potentially present throughout life and is manifested espe-cially by children and elderly people in stressful situations. The way in which and the person to whom this behavior is expressed changes over time (Miesen, 1990). Although Bowlby indicates that attachment be-havior is potentially present throughout a person’s lifetime, he has conducted no empirical research of at-tachment behavior during old age or in people with dementia.
Miesen applied attachment theory to elderly people who have dementia (1990, 1992, 1993). Based on clinical experience, Miesen concluded that every elderly person with dementia, at some point, appears to cling to the idea that his or her parents, who have long since died, are still alive (parent-fixation). This be-havior is expressed, among other things, by: the person with dementia expressing the desire to go home or to his or her parents and asking where their parents are (Miesen, 1993).
From the attachment theory perspective, this behavior not so much implies loss of memory, but might be an anxiety reaction because of experiencing the losses that accompany the dementia. In this way parent-fixation can be con-sidered an expression of the need for security (Miesen, 1990). Furthermore, it is possi-ble that the elderly person with dementia experiences the deterioration that accompanies the dementia as a strange and stressful situation, which also evokes attachment behavior.
Miesen tested this theoretical assumption about the attachment of elderly people with dementia in 1987 in a study among the residents of a psychogeriatric nursing home. Parent-fixation was found in two thirds of the residents involved in the study (N=40), and it was also found that the degree and the way in which parent-fixation exists is related to the stage of the dementia. Parent-fixation was exhibited especially by elderly people with dementia who had a low level of cognitive functioning (Miesen, 1993).
Coleman et al. (1997) examined whether a training course based on attachment theory for the staff of resi-dential homes had a positive effect on the staff members’ recognizing the emotional needs of the residents with dementia. In 18 training sessions, based on attachment theory, subjects such as dementia and depres-sion, communication with the person with dementia, and coping with behavior problems were addressed. This training course appeared to result in an increased response from staff members to signals from resi-dents aimed at getting attention, and in a decrease of the intensity of anxiety in the residents.
In The Netherlands, the principles of attachment theory are applied in the so-called ‘warm care’, an ap-proach that is similar to the ‘gentle care’ approach used in the United States and Canada (Jones & Wright, 1991). This approach focuses on offering a homelike, familiar and secure environment to elderly people with dementia (Houweling, 1987).
Adaptation-coping model
Dröes (1991, 1996, 1997b) developed the adaptation-coping model (1991, 1996, 1997b). The model offers a frame for explaining behavior problems in elderly people with dementia. One of the major presumptions of the adaptation-coping model is that people constantly strive for equilibrium. When people are con-fronted with changes in their existence, this will lead to a disruption of the balance. To regain balance, they will try to cope with these changes.
Dröes applied this general interactional principle formulated by Lazarus and Folkman (1984) to elderly people with dementia and added elements from Moos and Tsu’s (1977) crisis model which concentrates specifically on the adjustment of people in the case of serious illness. Moos and Tsu (1977) indicate that a number of general adaptive tasks are important for the restoration of the balance disrupted by serious ill-ness.
Elderly people with dementia can also be confronted with a disrupted balance as a result of the conse-quences of the illness. Dröes (1991) therefore assumes that the adaptive tasks mentioned by Moos and Tsu are also important to people with dementia. She names the following examples of cognitive adaptive tasks: learning to cope with the invalidity that is caused by the dementia and the development of an adequate re-lationship with the professional staff. Examples of emotional adaptive tasks are: preserving an emotional balance, preserving a positive self-image, and preparation for an uncertain future. She distinguishes the following social adaptive tasks: developing and maintaining social relationships and dealing with the nursing home environment and special treatment procedures (Dröes, 1997b).
Theoretically, the different adaptive tasks are distinguishable from each other, but, in reality, the way in which the person with dementia handles the adaptive tasks mentioned is, of course, a complex adaptation process (see Figure 3.3).
The degree to which an adaptive task is experienced as stressful depends on the cognitive appraisal of the situation or the change the elderly person with dementia is going through, either consciously or uncon-sciously. Personal factors, illness-related factors, and material and socioenvironmental factors affect this subjective appraisal. The adaptation-coping model views adjustment as an interactional, dynamic process that develops through an internal and an external cycle. The internal cycle takes place inside the person with dementia and may be viewed as a learning process. The external cycle concerns the interaction be-tween the elderly person with dementia and the environment (Dröes, 1991).
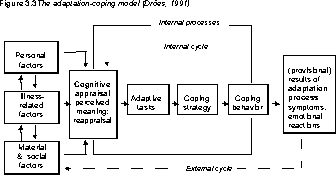
The application of the adaptation-coping model in psychogeriatrics offers possibilities for diagnosis, treat-ment, and evaluation of psychosocial problems in elderly people with dementia.
It is used in several psychogeriatric nursing homes in the Netherlands (Van der Kooy & De Ruiter, 1996), as well as in support programs for people with dementia who live at home and their central caregivers (Dröes & Breebaart, 1994; Dröes, 1996;1997a; Koens, 1997; Ladage, 1997; Projectgroep Gro-ningse Ont-moetingscentra, 1997). The model has been operationalized for application in psychomotor therapy (Dröes,1991; 1997b) and has proved to be a practicable theoretical framework for intervention research among people with dementia (Dröes, 1991; 1996).
The Dynamic system analysis model (DSA)
Bakker (1992, 1994, 1997) has applied a number of principles from the system-theory perspective (Von Bertanlanffy, 1974; Sipsma, 1988; Milders & Van Tilburg, 1988) to the situation of elderly people with dementia. He pre-sents a model that attempts dynamically to integrate psychosocial and somatic factors, as well as their continuous mutual interaction, and that involves psychologic, somatic, sociologic and life history factors (Bakker, 1992).
According to the dynamic system analysis (DSA) mental disorders in psychogeriatric patients are the result of an imbalance within the person, the environment, and the interaction between the two (Bakker, 1992; 1997). This imbalance results in a reduction or loss of autonomy and loss of the ability to realize a suitable environment. The relationship between cause and effect is not immediately obvious, there is a whole group of interrelated factors (the system). The important positive and negative factors that cause the psycho-geriatric disorder can vary per individual. That is why the significance of those factors in their mutual in-teractions (analysis) is examined on an indivi-dual basis. The analysis starts as much as possible from the way the person with dementia experiences and gives meaning to his or her environment. Intervening in specific factors in these cyclical processes can influence mental problems.
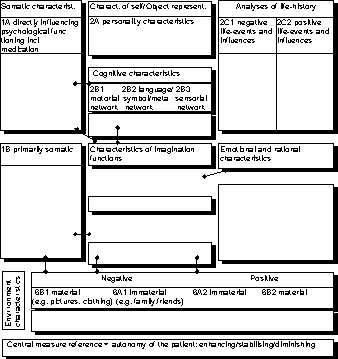
Based on an analysis scheme (see Figure 3.4) data on the various main functions and factors are invento-ried. In this way an attempt is made to map, as systematically as possible, every individual as a system, and gain insight into the processes and elements that have led to the psychogeriatric problems.
Filling in the scheme is a first step in the treatment process that takes place in a multidisciplinary manner and is based on the stages of the cyclical process of providing care from diagnosis through evaluation (Bakker, 1992).
The DSA-based treatment consists of a combination of medication, emotional support and a change in liv-ing environment. The model is used in a limited number of Dutch nursing homes as a starting point for the care and has been used there as a theoretical framework in a retrospective study of the effect of reactivation therapy for psychogeriatric patients (Bakker et al. in progress 1998).
The stages approach of Souren and Franssen
Souren and Franssen (1993a; 1993b) base their functional care method for people with Alzheimer’s disease primarily on the Functional Assessment Staging of Alzheimer’s disease (FAST) developed by Reisberg et al (1988). This assessment divides Alzheimer’s disease into four consecutive stages. The process of pro-viding care during the course of the illness in elderly people with Alzheimer’s disease has been divided into four stages that correspond with the different stages of illness (see Figure 3.5).
The illness and assistance stages constitute the framework of the so-called LIMIT-scheme (scheme of limitations). This is a practical instrument for people who take care of elderly persons with Alzheimer’s disease. The LIMIT-scheme makes it possible to assess what the person with dementia is still able to do and, in this way, arrive at a general care plan for the person with Alzheimer’s disease.
For each of the stages of the illness social-recreational, domestic and self-care activities are suggested. It also indicates for which of the activities the person with dementia needs encouragement or partial help, and which activities should be taken over completely. It also describes the attitude the caregiver can best adopt to achieve the desired result. The main objective is to keep the person with dementia active for as long as possible (Souren en Franssen, 1993a; 1993b).
Figure 3.5 Illness stages and stages of support for people with Alzheimer’s disease
(Souren en Franssen, 1993a)
| Illness stage | Stages of support |
| I. Loss of planning and initiative | Encouragement stage |
| II. Loss of insight, judgement and motivation | Intervention stage |
| III. Loss of learned everyday, more or less routine activities and speech |
Stage of partial taking over of activities |
| IV. Complete loss of spontaneous motor movement activity | Stage of complete taking over of activities |
Although loss of function is relatively predictable according to Souren and Franssen, the way in which the elderly person with dementia copes with this loss is not. Each person with dementia takes a different atti-tude with regard to the experienced losses. Behavior changes should be viewed as compensation mecha-nisms used by the person with dementia to regain balance (see also Dröes, 1991).
The caregivers of the person with dementia play an important role in this process of coping with functional loss. They must try to support the person with dementia in his or her process of illness by maintaining as much contact as possible with the person and by showing as much empathy as possible for the person’s situation. Offering affection is very important, because this will stay significant for the person with demen-tia, even when the environment has lost all significance (Souren and Franssen, 1993a).
Souren and Franssen’s ideas are based on their extensive practical experience with people with Alz-heimer’s disease and their involvement in a large-scale longitudinal study. This study observed five hun-dred people with Alzheimer’s disease from the beginning of the disease until the end of life (Souren and Franssen, 1993a; 1993b).
The Hagberg psychodynamic perspective
Hagberg (1997) advocates a psychodynamic approach to dementia. He views the behavior of people with dementia not only from the perspective of diagnosis and cognitive deterioration, but also from the life span perspective.
His approach is in line with the psychodynamic principles as described by Verwoerdt (1976, 1981). The Hagberg psychodynamic approach takes into consideration different variables (self-image, personality, ex-periences, ego functions and defense mechanisms) that together influence the functioning of the person with dementia. In this way, the course of the dementia can be anticipated. Changes in biologic processes, illness, cognition, and environment are thought to have an effect on coping and quality of life (see Figure 3.6).
Figure 3.6 Coping in a life-span perspective (Hagberg, 1997)

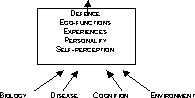
The model attempts to represent the relationship between the different varia-bles. It is based on the as-sumption that the person with dementia adjusts to the changes brought on initially by the dementia through an adaptive psychodynamic process, which is based primarily on earlier experiences and personal factors, such as personality and ego functions (see also Dröes, 1991).
The most important symptom of dementia is cognitive change. This has a far-reaching impact on general functioning. The person with dementia not only reacts to changes in cognitive functioning, but is also in-fluenced by them, for example in the capacity to process new experiences. Quickness of response, concen-tration, abstract thinking, and planning ability decrease, as do the available defense mechanisms.
Hagberg (1977) views the degree of cognitive deterioration based on three dimensions: cognitive powers, ego functions, and social relationships. He distinguishes five stages of cognitive deterioration, varying from: no cognitive disabilities to general deterioration accompanied by aphasia, apraxia, and agnosis. The various stages of cognitive deterioration are generally accompanied by certain dominant behaviors. Based on this, several approaches are suggested, such as: training, supporting, explaining, empathizing, and acti-vating. The care must focus on optimizing the adaptation.
The principles of the Hagberg psychodynamic approach are partly theoretical and partly based on the re-sults of the Lund Longitudinal Dementia Study (Hagberg, 1997). Hagberg advocates a practical application of this approach in the psychogeriatric field. We do not know if the Hagberg psychodynamic perspective is currently being used as a theoretical principle to care for elderly people with dementia.
| Model | Theoretical perspective | Starting point | Focus of care | Application | Research Care |
| Developmental stage model (Erikson, 1963) | Developmental theory |
Eight developmental stages with specific problems. Depending on how people cope they develop “strong” and “weak” characteristics | Foster positive results from psychosocial crises by offering environment that uses capacities of person with dementia optimally |
Study among nursing home residents with dementia |
Feil (1991) adds stage nine ‘resolution vs. vegetation’. ‘Integrity promoting care’ in nursing home residents with dementia |
| PLST model (Hall & Buckwalter, 1987) |
Coping theories Lazarus (1966) and Selye (1980), learning theory and physiological research | Phased course of DAT with lowering of stress tolerance threshold which increases changes of dysfunctional behavior | Modify environment to person’s stress tolerance threshold, f.e. by reduction of stimuli | Theoretical framework in nursing research | Basis for treatment programs and care plans for elderly with dementia at home and in institutions |
| Dialectical framework (Kitwood, 1989) | Biologic and psychologic principles; observational research, interviews with family | Dementia is a combination of neurologic and sociopsychologic factors. Psychologic environment is important to well-being | Approach person with dementia respectfully to limit deterioration in functions | Studies of the effect of psychologic environment on people with dementia | Unknown if model is used anywhere outside DCM studies conducted by Kitwood |
| Attachment theory (Miesen, 1990) |
Attachment theory (Bowlby, 1983) | Parent-fixation, possibly anxiety response to losses accompanying dementia | Offer familiar environment to reduce anxiety in person with dementia | Research of parent-fixation in dementia | Elements from attachment theory basis for ‘warm care’ |
| Adaptation-coping model (Dröes, 1991) | Coping model Lazarus and Folkman (1984) and adaptive tasks Moos and Tsu (1977) | Behavior pro-blems result from adaptation problems. Adaptation affected by environmental, illness, and personality factors | Support adaptation based on cyclical model for psychosocial care | Framework for research among people with dementia at home and in residential care | Principle in model for psychosocial care in intramural and extramural setting |
| Dynamic system Analysis (Bakker, 1992) | System theory | Mental disorders result from imbalance within person, environment and interaction between the two | Analyze indivi-dual as a system. Offer emotional support, modify environment and medication | Framework for retrospective study among people in the early stages of dementia | Theoretical framework for multidisciplinairy care in intramural setting |
| Stages approach (Souren & Franssen, 1993) | Biological approach; FAST (Reisberg et al. 1993) | Phased course of DAT and increasing loss of skills | Maintain activity of people with Alzheimer’s disease and support them through illness by offering affection | Applied in longitudinal study of people with Alzheimer’s disease |
Not used in the care, apart from the study mentioned (as fas as could be determined) |
| Psychodynamic model (Hagberg, 1997) | Psychodynamic theories, Lund longitudinal dementia study (Hagberg, 1997) | Cognitive change affects all aspects of being. Coping behavior related to diagnosis, social relations, person and experience | Optimize adaptation, based on diagnosis and personality of person | Model not yet applied in research, as far as could be determined | Not yet used in care as far as could be determined |
Conclusion and discussion
Based on an examination of the literature, the contents, background, and application of psychosocial mod-els used in the psychogeriatric field were addressed (see Table 3.7). Eight models were traced, all charac-terized by a focus on the individual and a multidimensional view of the behavior of people with dementia.
Although all of the described models may be called psychosocial and emotion- oriented, they also contain, in varying degrees, elements from the consequences model (see introduction). In other words: they also pay attention to compensating and limiting the functional consequences of dementia.
The theoretical background of the models (f.e., system theory, developmental theory, or psychodynamic theory), determines whether emphasis is placed on the consequences of the disease or on coping with the consequences of the disease. Examples are: attachment theory, the progressively lowered stress threshold model, the Kitwood dialectical framework and the LIMIT scheme. These models attach great importance to the modification of the psychosocial and/or material environment of the person with dementia, to compensate for his deteriorating mental functions.
The majority of the models consider the dementia and the accompanying changes in cognitive functioning as the main determinants and, unfortunately, as unalterable factors in the behavior of the person with de-mentia. None of the described models start from a medical perspective, in the sense that they focus on tracing the cause of the disease to cure it. Integration of the perspectives of the medical model, the conse-quences model, and the psychosocial model is expressed most explicitly in the dynamic system analysis model.
We wonder to what extent the models described here may serve as a starting point for emotion-oriented care for people with dementia syndromes, more specifically Alzheimer’s disease, and to what extent may serve as a theoretical framework for research into this type of care. To answer this question we use the fol-lowing criteria: the degree to which the model has been operationalized and offers points of departure for psychogeriatric care, the degree to which the model has been subjected to empirical testing and the target group for which the model was developed.
Operationalization of the model for psychogeriatrics
The degree to which the models have been operationalized and offer concrete starting points for the provi-sion of care varies. The Erikson developmental stage model and attachment theory do not offer concrete leads for the care provision, but they have been operationalized for psychogeriatrics. Feil (1967, 1984, 1989) has added a ninth stage to the Erikson developmental stage model to accommodate people with de-mentia. Kihlgren et al. (1996) examined the suitability of the theory for application as a theoretical frame-work in ‘integrity promoting care’ for nursing home residents with dementia. The limited operationaliza-tion of especially the ‘weak’ characteristics has proved to be an important shortcoming of the develop-mental stage model.
Miesen (1990) tested the attachment theory on people with dementia. However, attachment theory explains only one aspect of the behavior of elderly people with dementia, i.e. parent-fixation. In our opinion, this renders the attachment theory unsuitable as a general theoretical frame for the total psychosocial care in dementia. The other models consider the behavior of the person with dementia in a more general way and are, therefore, more suitable as starting points for the care provision. The LIMIT scheme of Souren and Franssen and the Kitwood dialectical framework offer the most detailed suggestions of how to approach and support people with dementia and provide care to them. Three of the other models, i.e. the adaptation-coping model, the dynamic system analysis and the progressively lowered stress threshold model, have furthermore been elaborated into concrete instructions for the entire cyclical care process from diagnosis, when establishing the request for help is the central issue, through evaluation. These models have been op-erationalized at the behavioral level, and have also been used in research. For now, we recommend that practitioners or researchers use one of these three models.
Empirical verification
As far as we know, the validity of only the attachment theory (Miesen, 1990) has been tested empirically. With the adaptation-coping model, only the different adaptive tasks have been tested so far (Dröes, 1991). Currently, the model as such is being tested in a group of psychogeriatric nursing home residents. There-fore, in general, we must conclude that the degree of validity of the models previously described is not clear.
Empirical verification of a model is of importance in a research setting, but from the caregiver’s perspec-tive, this may be less important than its practicability. This practicability is naturally linked to the degree to which the model can be operationalized for the care setting. As we observed earlier, opera-tionalization and application proved possible for the majority of the models described. Only with regard to the Hagberg (1997) psychodynamic perspective does it remain unclear whether this perspective has already been ap-plied to the care practice and to the study of people with dementia.
Target group
The target groups for which the models were developed also vary. The progressively lowered stress thresh-old model, the adaptation-coping model, and the LIMIT scheme were originally developed for people with a probable diagnosis of Alzheimer’s disease or a related disorder. Hagberg and Kitwood developed their model for a broader group, i.e. persons with different types of dementia (including frontal lobe dementia, vascular dementia, and Alzheimer’s disease). The other models were developed for psychogeriatric patients in the broad sense of the term, not for a specific diagnostic group.
It is obvious that a fitting theoretical framework is essential for providing emotion-oriented care to people with dementia. Because most models are quite recent and have not yet been subjected to empirical testing, it is too early to judge their theoretical validity. Practitioners will prefer those models that are operational-ized for home care or institutional care, and have already been found suitable for the target group.
The progressively lowered stress threshold model, the adaptation-coping model, and the dynamic system analysis model meet the requirement of clear operationalization, the first two being for both home care and institutional care, and the dynamic system model being only for institutional care. They offer concrete in-structions for the entire cyclical care process. That is why, for now, the use of one of these models is rec-ommended as a basis for emotion-oriented care.
The challenge for future research is the empirical testing of the models to advance the development of knowledge in the care of people with dementia. So far, only the attachment theory has been tested. Fur-thermore, a start has been made with the empirical testing of the adaptation-coping model.
For a model to be tested, it needs to be operationalized clearly. For most of the psychosocial models de-scribed this seems to be the case. An exception is the Erikson developmental model, which lacks clear definitions of especially the ‘weak’ characteristics. Finally, evaluation research can be fruitful to test the ef-fect of interventions resulting from the psychosocial models on people with dementia with regard to main-taining an optimal quality of life.
If the models withstand empirical scrutiny, they can truly provide a systematic structure for thinking, for observations, and for interpreting what is seen. Furthermore, they can give a rationale for activities and point out solutions to practical problems (Fawcett, 1989).
References
American Psychiatric Association (1997). Practice guidelines for the treatment of patients with Alzheimer's disease and other dementias of late life. American Journal of Psychiatry, 154[Suppl 5], 1-39.
Atkinson RL, Atkinson RC, Smith EE, Bem DJ & Hilgard ER (1990). Psychological development. In: RL Atkinson, RC Atkinson, EE Smith, DJ Bem & ER Hilgard (Eds), Introduction to psychology (10 ed., pp. 108-113). San Diego, USA: Harcourt Brace Jovanovich Inc.
Bakker TJEM (1992). Integrale psychogeriatrie in de praktijk: diagnose en behandelingop basis van een dynamische systeem analyse. Amsterdam/Lisse: Swets & Zeitlinger BV.
Bakker TJEM (1997). Psycho-geriatrie behandelpraktijk in meer dimensies, diagnose en behandeling met dynamische systeem analyse. Lisse: Swets & Zeitlinger BV.
Bakker TJEM, Duivenvoorden HJ & Schudel WJ (concept1998). Psycho-geriatrische reactivering in het verpleeghuis.
Bakker TJEM, Lit AC & Schroots JJF (1994). Naar een nieuwe psychogeriatrie, pluriform en complex. Lisse: Swets & Zeitlinger BV.
Baltes MM & Barton EM (1979). Behavioral analysis of aging: a review of the operant model and re-search. International Journal of Behavioral Development, 2(3), 297-320.
Bowlby J (1983). Verbondenheid. Deventer: Van Loghum Slaterus.
Butler RN (1963). The life review: An interpretation of reminiscence in the aged. Psychiatry, 26, 65-76.
Cohen D (1991). The subjective experience of Alzheimer's disease: The anatomy of an illness as perceived by patients and families. American Journal of Alzheimer's Care and Related Disorders & Research, 6, 6-11.
Coleman P, Conroy C, Jerrome D, Meade R, Mills M (1997). Changing patterns of dementia care through staff training: the effects of a course with draws on attachment theory. 1st Bologna international meeting on cognitive and affective disorders in the elderly. Bologna, Italy, June 19-21.
Collins JA, Crump S, Buckwalter KC, Hall GR, Gerdner LA & Kudart P (1995). Uncovering and manag-ing denial during the research process. Archives of Psychiatric Nursing, 9(2), 62-67.
Cotrell V & Lein L (1993). Awareness and denial in the Alzheimer's disease victim. Journal of Geron-tological Social Work, 19(3/4), 115-132.
Cotrell V & Schultz R (1993). The perspective of the patient with Alzheimer's disease: a neglected dimen-sion of dementia research. The Gerontologist, 33(2), 205-211.
Dröes RM (1991). In beweging: over psychosociale hulpverlening aan demente ouderen. Utrecht: De Tijdstroom.
Dröes RM (1995). Psychosociale behandeling bij dementie. Tijdschrift voor Psychiatrie, 37(3), 235-260.
Dröes RM (1996). Amsterdamse ontmoetingscentra: een nieuwe vorm van ondersteuning voor dementer-ende mensen en hun verzorgers, Eindrapport. Amsterdam: Thesis Publishers.
Dröes RM (1997). Amsterdamse ontmoetingscentra, een ondersteuningsprogram-ma voor thuiswonende dementerenden en hun verzorgers in buurtcentra. In: Handboek dagbesteding (pp. c4220-1 t/m 28). Houten: Bohn Stafleu Van Loghum.
Dröes RM (1997). Psychomotor group therapy for demented patients in the nur-sing home. In: BML Mie-sen & GMM Jones (Eds), Care-giving in dementia, research and applications Volume 2 (pp. 95-118). London/New York: Routledge.
Dröes RM & Breebaart E (1994). Amsterdamse ontmoetingscentra: een nieuwe vorm van ondersteuning voor dementerende ouderen en hun verzorgers, Voorstudie. Amsterdam: Thesis Publishers.
Erikson EH (1963). Childhood and Society. London: Imago Publishing Co. Ltd.
Fawcett J (1989). Analysis and evaluation of conceptual models of nursing. Philadelphia: FA Davis Com-pany.
Feil N (1967). Group therapy in a home for the aged. The Gerontologist, 7(3), 192-195.
Feil N (1984). Communicating with the confused elderly patient. Geriatrics, 39, 131-132.
Feil N (1989). Validation: an empathic approach to the care of dementia. Clinical Gerontologist, 8(3), 89-94.
Feil N (1992). Validation therapy with late-onset dementia populations. In: GMM Jones & BML Miesen (Eds), Care-giving in dementia, research and applications (pp. 199-218). London/New York: Tavistock/ Routledge.
Feil N & Klerk-Rubin V de (1991). Vraagtekens bij validation? Een reactie op 'Ervaringen met validation' van Verdult en Visser - TvZ nr. 15, 1990. TvZ / Vakblad voor Verpleegkundigen, 101(2), 44-46.
Finnema EJ, Dröes RM, Ribbe MW & Tilburg W van (1998). The design of a large-scale experimental study into the effect of emotion-oriented care on demented elderly and professional carers in nursing homes. Archives of Gerontology and Geriatrics [Suppl 6], 193-200.
Fruehwirth SE (1989). An application of Johnson's behavioral model: a case study. Journal Community Health Nursing, 6(2), 61-71.
Gerdner LA, Hall GR & Buckwalter KC (1996). Caregiver training for people with Alzheimer's based on a stress threshold model. IMAGE: the Journal of Nursing Scholarship, 28(3), 241-246.
Gerdner LA, Stolley JM, Hall GR, Garand L & Buckwalter KC (1996). Nursing care of patients with de-mentia. In: MF Weiner (Ed), The dementias: diagnosis, management, and research (2 ed., pp. 281-296). Washington DC: American Psychiatric Press Inc.
Hagberg B (1997). The dementias in a psychodynamic perspective. In: BML Miesen & GMM Jones (Eds), Care-giving in dementia, research and applications Volume 2 (pp. 14-35). London/New York: Rout-ledge.
Hagberg B & Gustafson L (1985). On diagnosis of dementia: psychometric investigation and clinical psy-chiatric evaluation in relation to verified diagnosis. Archives Gerontol. Geriatr., 4, 321-332.
Hall GR (1988). Care of the patient with Alzheimer's disease living at home. Nursing Clinics of North America, 23(1), 31-45.
Hall GR (1994). Caring for people with Alzheimer's disease using the conceptual model of progressively lowered stress threshold in the clinical setting. Nursing Clinics of North America, 29(1), 129-141.
Hall GR & Buckwalter KC (1987). Progressively lowered stress threshold: a conceptual model for care of adults with Alzheimer's disease. Archives of Psy-chiatric Nursing, 1(6), 399-406.
Hall GR & Buckwalter KC (1991). Whole disease care planning: fitting the program to the client with Alz-heimer's disease. Journal of Gerontological Nursing, 17, 38-41.
Hall GR, Buckwalter KC, Stolley JM, Gerdner MA, Garand L, Ridgeway S & Crump S (1995). Standard-ized care plan managing Alzheimer's patients at home. Journal of Gerontological Nursing, 37-49.
Hall GR, Gerdner L, Szygart-Stauffacher M & Buckwalter KC (1995). Principles of nonpharmacological management: Caring for people with Alzheimer's disease using a conceptual model. Psychiatric Annals, 25(7), 432-440.
Hetherington EM & Parke RD (1993). Chapter 1 Introduction: Themes and theories. In: EM Hetherington & RD Parke (Eds), Child psychology a contemporary viewpoint (4 ed., pp. 1-28). New York: McGraw-Hill inc.
Houweling H (1987). Warme zorg, een visie op psychogeriatrische zorgverlening. Tijdschrift voor be-jaarden- ,kraam- en ziekenverzorgenden, 20(2), 39-42.
Jones G (1992). A communication model for dementia. in: GMM Jones & BML Miesen (Eds), Care-giving in dementia, research and applications (pp.76-99). London/New York: Routledge.
Jones G & Burns A (1992). Reminiscing disorientation theory. in: GMM Jones & BML Miesen (Eds), Care-giving in dementia, research and applications (pp.57-76). London/New York: Routledge.
Jones MJD & Wright J (1991). Beyond love a resource book for caregivers support and education. Burnaby: Moyra Jones resources.
Kihlgren M, Hallgren A, Norberg A & Karlsson I (1996). Disclosure of basic strengths and basic weak-nesses in demented patients during morning care, before and after staff training: analysis of video-recordings by means of the Erikson theory of "Eight stages of man". Int'l. J. Aging and Human Develop-ment, 43(3), 219-233.
Kitwood T (1989). Brain, mind and dementia: with particular reference to Alzheimer's Disease. Ageing and Society, 9, 1-15.
Kitwood T (1990). The dialectics of dementia: with particular reference to Alzheimer's Disease. Ageing and Society, 10, 177-196.
Kitwood T (1993a). Person and process in dementia. International Journal of Geriatric Psychiatry, 8, 541-545.
Kitwood T (1993b). Towards a theory of dementia care: the interpersonal process. Ageing and Society, 13, 51-67.
Kitwood T (1996). A dialectical framework for dementia. In: RT Woods (Ed), Handbook of the clinical psychology of ageing (pp. 267-282). Chichester, England: John Wiley & Sons Ltd.
Kitwood T (1997). The concept of personhood and its relevance for a new culture of dementia care. In: BML Miesen & GMM Jones (Eds), Care-giving in dementia, research and applications Volume 2 (pp. 3-13). London/New York: Routledge.
Kitwood T (1998). Toward a theory of dementia care: ethics and interaction. Journal of Clinical Ethics 9, 23-34.
Kitwood T & Bredin K (1992). A new approach to the evaluation of dementia care. Journal of Advanced Health Nursing Care, 1 (5), 41-60.
Kitwood T & Bredin K (1994). Evaluating dementia care: The DCM method (6 Ed). Bradford: Bradford Dementia Research Group.
Kiyak HA & Borson S (1992). Coping with chronic illness and disability. In: MG Ory, RP Abeles & PD Lipman (Eds), Aging, health and behavior (pp.141-173). London: Sage Publications.
Koens J (1997). Het huis in de wijk, een kleinschalige voorziening voor demen-terende ouderen in Alk-maar-Zuid. Alkmaar: Stichting Westerhout.
Kolanowski AM & Whall AL (1996). Life-span perspective of personality in dementia. IMAGE: Journal of Nursing Scholarship, 28(4), 315-320.
Kooij C van der & Ruyter M de (1996). Invoering van het integrale zorgdossier. Nieuwe vormen van multi-disciplinair overleg in de verpleeghuiszorg. Utrecht: NZi.
LadageJP (1997). Projectplan: ondersteuningsprogramma voor dementerende ouderen en hun verzorgers in Amstelveen. Amstelveen/Uithoorn: Stichting Welzijn Ouderen.
Lazarus RS & Folkman S (1984). Stress, appraisal and coping. New York: Springer Publishing Company.
Levy LL (1987). Psychosocial intervention and dementia: II. The cognitive disability perspective. Occupa-tional Therapy in Mental Health, 7(4), 13-36.
Levy LL (1987). Psychosocial intervention and dementia, Part I: State of the art, future directions. Occu-pational Therapy in Mental Health, 7(1), 69-107.
Matteson MA, Linton AD & Barnes SJ (1996). Cognitive developmental approach to dementia. IMAGE: Journal of Nursing Scholarship, 28(3), 233-240.
Miesen BML (1990). Gehechtheid en dementie. Ouders in de beleving van dementerende ouderen. Almere: Versluys.
Miesen BML (1992). Attachment theory and dementia. In: GMM Jones & BML Miesen (Eds), Care-giving in dementia, research and applications. London/ New York: Tavistock/Routledge.
Miesen BML (1993). Alzheimer's disease, the phenomenon of parent fixation and Bowlby's attachment theory. International Journal of Geriatric Psychiatry, 8, 147-153.
Milders CFA & Tilburg W van (1988). Systeemdenken & psychiatrie, een kritische oriëntatie. Assen/ Maastricht: Van Gorcum.
Moore I (1997). Living with Alzheimer's: understanding the family's and patient's perspective. Geriatrics, 52 [Suppl 2], 33-36.
Moos RH & Tsu VD (1977). The crisis of physical illness: an overview. In: RH Moos (Ed), Coping with physical illness (pp. 3-21). New York/London: Plenum Medical Book Company.
Prins AAM (1993). The case of untraceable Alzheimer patients: medical practices and intellectual tradi-tions of psychiatrists and geriatrists in the Netherlands 1900-1988. In: I Lowy (Ed), Medicine and change: historical and sociological studies of medical innovation (pp. 395-419). London: John Libbey Eurotext.
Projectgroep Groningse Ontmoetingscentra (1997). Projectvoorstel zorgver-nieuwing Groningse ontmoet-ingscentra: een nieuwe vorm van ondersteuning voor dementerende mensen en hun mantelzorgers. Groningen: verpleeghuis Innersdijk/Stichting Welzijn in Groningen.
Rabins P (1994). The phenomenology of behavior: an overview of behavioral principles. Alzheimer's Dis-ease and Associated Disorders, 8(Suppl. 3), 61-65.
Reisberg B, Franssen EH, Borenstein J & Ferris SH (1988). Functional assessment staging (FAST). Psy-chopharmacological Bulletin, 24, 653-659.
Sipsma DH (1988). Sociale geriatrie en de geriatrische patiënt. In: WJA Goedhard & DL Knook (Eds), Geriatrie-informatorium (pp. F2005-1 t/m 27). Houten/ Antwerpen: Bohn Stafleu Van Loghum.
Souren L & Franssen E (1993). Verbroken verbindingen: de ziekte van Alzheimer deel I - Ontstaan en ver-loop. Amsterdam/Lisse: Swets & Zeitlinger BV.
Souren L & Franssen E (1993). Verbroken verbindingen: de ziekte van Alzheimer deel II - Praktische richtlijnen voor het omgaan met de Alzheimerpatiënt. Amsterdam/Lisse: Swets & Zeitlinger BV.
Spaull D & Leach C (1998). An evaluation of the effects of sensory stimulation with people who have de-mentia. Behavioural and Cognitive Psychotherapy, 26(1), 77-86.
Stokes G (1996). Challenging behavior in dementia: a psychological approach. In: RT Woods (Ed), Hand-book of the clinical psychology of ageing (pp. 601-628). Chichester, England: John Wiley & Sons Ltd.
Taft LB, Fazio S, Seman D & Stansell J (1997). A psychosocial model of dementia care: theoretical and empirical support. Archives of Psychiatric Nursing, XI(1), 13-20.
Thornbury JM & King LD (1992). The Roy adaptation model and care of persons with Alzheimer's dis-ease. Nursing Science Quarterly, 5(3), 129-133.
Verwoerdt A (1976). Clinical geropsychiatry. Baltimore: The Williams & Wilkins Co.
Verwoerdt A (1981). Individual psychotherapy in senile dementia. In: NE Miller & GD Cohen (Eds), Ag-ing (Vol. 15). New York: Raven Press.
Von Bertalanffy L (1974). General systems theory and psychiatry. In: S Arieti (Ed), American handbook of Psychiatry (2 ed., Vol. 1pp. 1095-1121). New York: Basic Book.
Whall AL (1989). Communicating with advanced-stage dementia patients: the application of Sullivanian theory. Journal of Gerontological Nursing, 15(9), 31-2.
Zinder M (1984). Senile dementia - reflections on rehabilitation procedures. In: J Wertheimer & Marois (Eds), Senile dementia: outlook for the future. New York: AR Liss Inc.
* Address of correspondence:
Evelyn Finnema, Utein 93, 9244 AA Beetsterzwaag, the Netherlands,
e-mail: kuifin@freeler.nl